 
While a small group of bacterial meningitis patients have CSF findings that mimic viral meningitis, clinicians should be able to apply the usual criteria in the majority of cases to differentiate between bacterial and viral etiology in those pretreated with antibiotic(s). Pretreatment with antibiotics diminished the CSF culture positive rate from 95% to 68% in one study ( 8). Although fewer patients were studied than for Hib, similar CSF findings were described for pneumococcal meningitis cases, but findings were less consistent in meningococcal meningitis ( 7– 9). However, antibiotic pretreatment led to a significantly lower mean CSF protein concentration (1.37 g/L versus 2.08 g/L) and rate of positive Gram stain (84% versus 92%, respectively) ( 6). In this study, the CSF total WBC count, percentage of neutrophils, glucose concentration and culture positivity rate did not differ significantly between previously treated and untreated groups ( 6). In one study, the mean CSF WBC count in patients with Hib meningitis previously treated with antibiotics was 5235×10 6/L (with 84% neutrophils), while the CSF to serum glucose ratio was 0.28 and mean CSF protein 1.37 g/L CSF Gram stain revealed bacteria in 84% ( 6). In partially treated bacterial meningitis, the CSF WBC counts and protein levels are typically higher than was found in the case scenario ( 5). A relatively low WBC count and mildly elevated protein in the CSF are consistent with viral infection ( 4), but one cannot completely rule out bacterial etiology because there have been bacterial meningitis cases without significant CSF pleocytosis ( 5). Modest hypoglycorrhachia has also been reported, occuring in up to 18% of enteroviral meningitis ( 3) and about one-quarter of mumps meningitis. For example, neutrophilic pleocytosis was found in up to two-thirds of cases of enteroviral meningitis ( 2). The neutrophil predominance in the CSF is not unusual early in viral meningitis. However, viral etiology was still most likely for two reasons. The major concern regarding the patient described in the case scenario was the possibility of partially treated bacterial meningitis (because of the prior amoxicillin use, the predominance of neutrophils in the initial CSF and the CSF glucose being less than 50% of the serum glucose). Is the initial CSF profile suggestive of a viral or bacterial etiology for the meningitis? 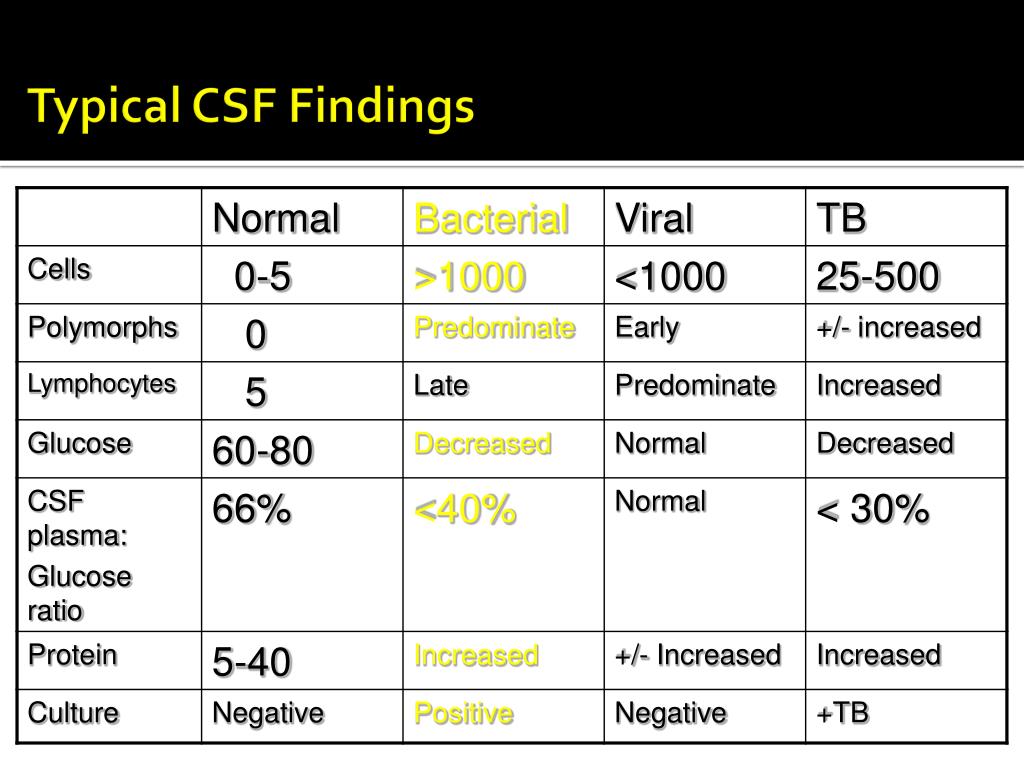
The child was seen two weeks later, and had a normal neurological examination. Three days later, an enterovirus was isolated from both CSF and stool culture, later confirmed to be an echovirus strain. This shift from predominantly neutrophilic to lymphocytic pleocytosis was most consistent with viral meningitis, and the child was discharged home. The CSF protein was 0.85 g/L and CSF glucose 3.5 mmol/L. The decision was made to repeat the lumbar puncture, which now showed a total CSF WBC of 380×10 6/L, with 70% lymphocytes. There were no positive blood and CSF bacterial cultures, and it was too early for viral culture results. Twenty-four hours later, the child had improved clinically. Throat swab and stool specimen were also sent for viral culture. Blood culture, and bacterial and viral cultures of CSF were sent for study. Parenteral antibiotic therapy was not initiated, and the oral antibiotic was discontinued. CSF latex agglutination tests for Streptococcus pneumoniae, Hib, Neisseria meningitidis serogroups A, C, Y and W-135, and N meningitidis serogroup B/ Escherichia coli K1 were negative. CSF protein 0.78 g/L (normal 0.15 to 0.4 g/L) and CSF glucose 2.6 mmol/L (simultaneous blood glucose level of 5.3 mmol/L). CSF white blood cell (WBC) count was 420×10 6/L, with 80% neutrophils, 15% lymphocytes and 5% monocytes. Initial lumbar puncture revealed cloudy cerebrospinal fluid (CSF), and Gram stain showed moderate neutrophils but no bacteria. No rash was evident, and there were no swollen or painful joints. There were no enlarged cervical nodes, nor signs of hepatosplenomegaly. Tympanic membranes and pharynx appeared normal. Rectal temperature was 39.5☌, heart rate was 126 beats/min and respiratory rate was 24 breaths/min. He was lethargic and had nuchal rigidity. He was immunized previously with four doses of diphtheria- tetanus-acellular pertussis-polio- Haemphilius influenzae b (DTaP-polio-Hib) and a single dose of measles, mumps and rubella (MMR) at 12 months. He was prescribed amoxicillin two days before, and had taken six doses in total. There were no prodromal symptoms, no infectious contacts, no pets at home and no recent travels. A two-year-old boy presented to an emergency room in July with a two-day history of fever, nausea and vomiting. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
